20 minutes to address 8 clinical problems
Depression and cPTSD do not present as one problem. They arrive as panic attacks, nightmares, insomnia, isolation, low self-worth, and financial collapse — all at once, all in the same consultation.
Your patient has depression and cPTSD. Behind that are panic attacks, nightmares, insomnia, social isolation, collapsed self-worth, distorted thinking, no job, and no financial safety net. Caredevo dissects every problem — and gives each one a goal, a task, and a referral.
This is not a faster consultation note creation. This is a structured care plan that actually maps the clinical reality.
No credit card required

The real picture
The standard MHCP misses most of what needs addressing.
What Caredevo does
A care plan that actually maps the clinical reality of complex mental health.
Reviews that mean something
Every 6-session review starts with a structured plan, not a blank page.
The consultation that cannot hold everything
Elizabeth is 52. She was diagnosed with depression and cPTSD following years of domestic abuse. She has not worked in eighteen months. She wakes three times a week from nightmares. She has not left her flat alone in six weeks. Her self-worth is near zero. She is surviving on JobSeeker with growing credit card debt.
The consultation runs 25 minutes. The GP listens carefully, assesses risk, prescribes an SSRI, and writes a referral to a psychologist. The MHCP lists the diagnosis. The referral mentions depression and trauma. Elizabeth leaves with an appointment and no map.
The psychologist receives a referral letter. They do not know about the panic attacks, the insomnia, the financial crisis, or the job situation. They start from scratch. Elizabeth explains everything again.
What was in that consultation — and never made it into the plan
Each of these is a clinical problem. Each deserves a goal. None of them made it into the MHCP.
Why this keeps happening
The problem is not the GP. It is a form that was not designed for clinical complexity — and a workflow that does not have time to fill the gap manually.
Depression and cPTSD do not present as one problem. They arrive as panic attacks, nightmares, insomnia, isolation, low self-worth, and financial collapse — all at once, all in the same consultation.
The standard MHCP refers to a psychologist. It does not name each problem, set goals for each, or coordinate who is responsible for what. The patient leaves with a referral and no roadmap.
Unemployment and financial stress worsen depression and derail recovery. But they are rarely documented with clinical goals and referrals. They exist in the consult, then disappear from the notes.
At the 6-session review, the GP re-establishes context rather than measuring progress. Without a structured problem breakdown, there is no shared thread between consultations.
The cost of an incomplete plan
When only the diagnosis is named, the psychologist works without context. The social worker never gets called. The financial crisis quietly deepens. The panic attacks continue untouched because they were never named as a separate problem with a separate goal.
Recovery from complex trauma is not linear. But it is also not random. It requires a structure that names every problem, coordinates every intervention, and tracks every goal across every review. Without that structure, clinicians work in silos — and patients fall through the gaps between them.
What a standard MHCP misses
Elizabeth — 52 yo, depression and cPTSD
This is what a problem-level MHCP looks like. Each presenting issue named, dissected, and given its own clinical direction.
Goal
Reduce frequency and severity of panic episodes using evidence-based grounding and breathing techniques within 8 weeks.
Tasks
Referral
Goal
Reduce frequency and distress of trauma-related nightmares and intrusive re-experiencing within 12 weeks.
Tasks
Referral
Goal
Establish consistent sleep onset within 30 minutes and reduce nocturnal waking to no more than once per night within 6 weeks.
Tasks
Referral
Goal
Increase meaningful social contact from near-zero to at least two interactions per week within 10 weeks.
Tasks
Referral
Goal
Build self-compassion and begin to challenge core shame-based beliefs within 12 weeks.
Tasks
Referral
Goal
Identify at least three recurring cognitive distortion patterns and apply restructuring techniques consistently within 8 weeks.
Tasks
Referral
Goal
Establish a supported vocational pathway — whether return-to-work, study, or voluntary activity — within 16 weeks.
Tasks
Referral
Goal
Stabilise financial situation through appropriate government support, concession entitlements, and financial counselling within 4 weeks.
Tasks
Referral
Why this level of structure matters
Each problem above was present in Elizabeth's consultation. Without naming each one, none of them become actionable goals. They stay as background noise in a diagnosis.
What this gives the psychologist
A structured handover that names every problem, every goal, and every agreed task — so session one starts with context, not re-assessment.
What this gives the GP
A framework for every follow-up consultation — to measure progress against named goals and identify which problems still need attention.
Caredevo vs other AI scribes
Standard AI scribes reduce typing. Caredevo structures the clinical picture — breaking the presentation into problems, goals, tasks, and referrals that every treating clinician can follow.
Faster consultation notes
Faster referral letter to psychologist
Structured presenting issue breakdown
Individual goal per clinical problem
Tasks and interventions per problem area
Referral mapped to each problem
Psychosocial problems documented with goals
6-session and 10-session review framework
Coordinated care across GP, psychologist, social worker
Standard AI scribes are built for one consultation. Caredevo is built for the patient's recovery journey.
How Caredevo works
Caredevo does not replace your clinical judgement. It gives you the structure to make every problem visible, every goal named, and every referral coordinated.
Capture the consultation by recording, dictating, Smart Paste, or typing. Caredevo builds one structured consultation note.
Each presenting issue — panic, nightmares, insomnia, isolation, self-esteem, cognition, employment, finances — gets its own clinical entry.
Every problem has a named goal, specific tasks and interventions, and a referral to the right clinician or service.
The problem breakdown becomes the thread across the 6-session and 10-session reviews. Progress is measured. Goals evolve. The plan stays alive.
Platform features
Caredevo dissects the mental health presentation into individual clinical problems — each with a goal, tasks, and referral — turning the MHCP from a referral letter into a genuine care framework.
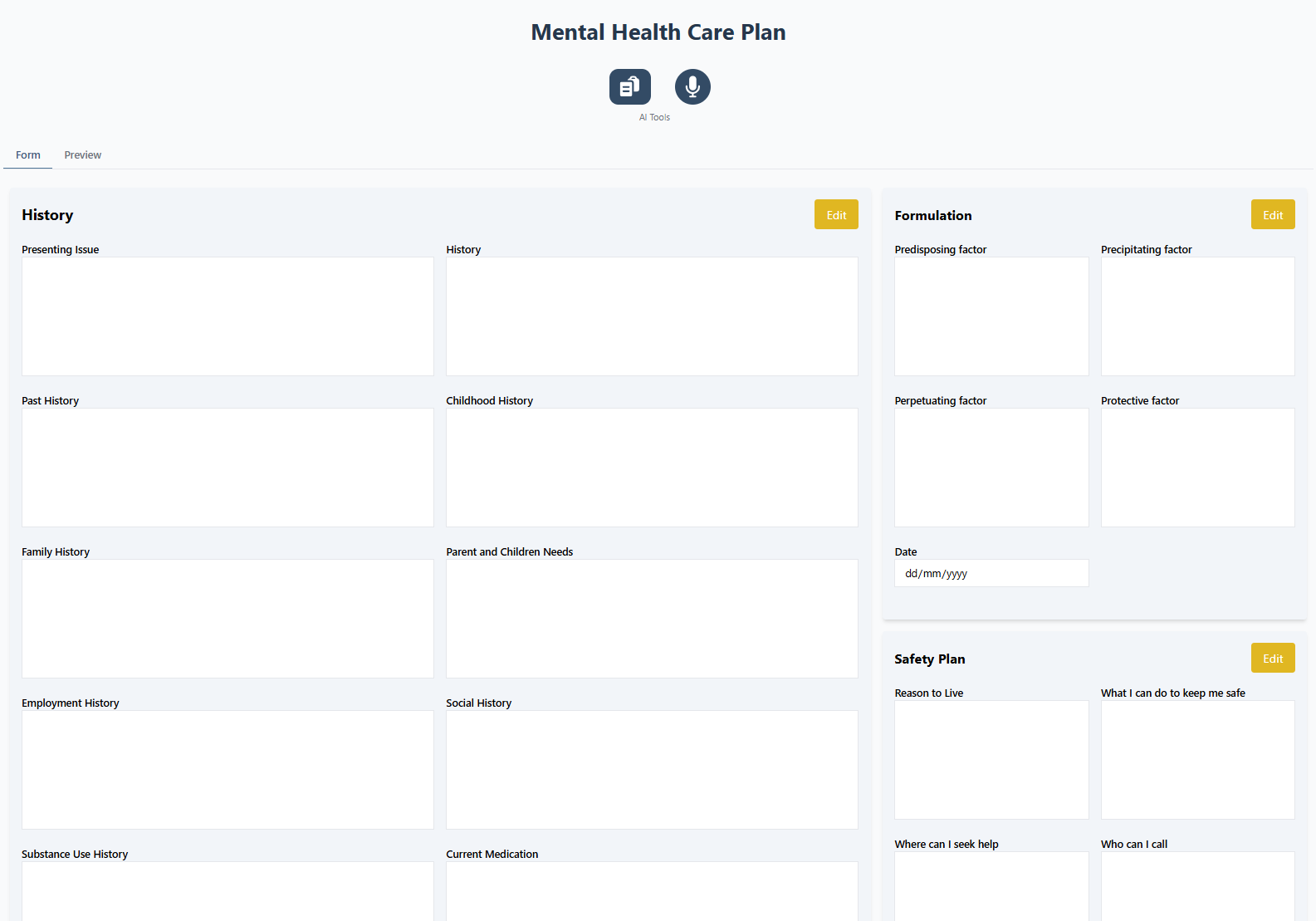
Why GPs choose Caredevo for mental health care planning
Example structured output — Elizabeth
Consultation
52-year-old female, depression and cPTSD following domestic abuse, 18 months unemployed, social isolation, financial stress
MHCP — individual problems
8 presenting problems each with named goal, tasks, and referral — panic, nightmares, insomnia, isolation, self-esteem, cognition, employment, finances
Referrals generated
Psychologist (trauma-focused CBT / EMDR), social worker, DES, financial counsellor
Review framework
6-session and 10-session review structure with problem-level progress markers already set
Caredevo is an assistant tool only. Final clinical judgement and documentation remain yours.
Ready to try it?
Turn one consultation into a structured MHCP — each presenting issue dissected, each goal named, each referral coordinated across the treating team.
No credit card required.
Answers for GPs considering Caredevo for structured mental health care planning.